Conventional Treatment Options
There is no guaranteed way of preventing piles, but a high fibre diet is a good place to start. This will reduce the risk of constipation and the straining to pass a stool that can cause haemorrhoids.
General recommendations are:
- Eat plenty of fresh fruit and vegetables (at least five portions every day)
- Cut down on fat (especially animal fat), sugary food, refined and processed food
- Eat plenty of pulses (eg peas, beans, lentils)
- Eat plenty of wholegrain foods (use the wholemeal varieties of bread, pasta and breakfast cereals)
- Drink alcohol in moderation
A high-fibre diet is also best if you already have haemorrhoids. This helps to prevent constipation and avoid the straining to pass a stool that can make haemorrhoids worse.
For most people with haemorrhoids, the condition is mild and can be treated with over the counter (OTC) medicines that tackle the symptoms, usually in the form of ointments or suppositories. Haemorrhoids caused by pregnancy may go away after the baby has been born. Various preparations and brands are commonly used. They do not ‘cure’ haemorrhoids. However, they may ease symptoms such as discomfort and itch.
A bland soothing cream, ointment, or suppository may ease discomfort. They can be used as often as you like. Several brands are available without a prescription. One that contains an anaesthetic may ease pain better. You should only use these for short periods at a time (5-7 days). If you use it for longer, the anaesthetic may irritate or sensitise the skin around the anus. One that contains a steroid may be prescribed by a doctor if there is a lot of inflammation around the haemorrhoids.
Steroids reduce inflammation and may help to reduce any swelling around a haemorrhoid. This may help to ease itch and pain. You should not normally use these for longer than one week at a time. Very painful prolapsed haemorrhoids are uncommon. The pain may be eased by an ice pack (or bag of frozen peas) pressed on for 15-30 minutes. Strong painkillers may be needed.
Haemorrhoids of pregnancy usually settle after the birth of the child. Treatment is similar to the above.
Injection Sclerotherapy
Injection of a ‘sclerosing’ (shrinking) chemical into the haemorrhoid, may be successful but the benefit is sometimes only short lived and may need to be repeated a few times.
Banding Treatment
This procedure is usually done by a surgeon in an outpatient clinic. A pile is grasped by the surgeon with forceps or a suction device. A rubber band is then placed at the base of the pile. This cuts off the blood supply to the pile which then ‘dies’ and drops off after a few days. The tissue at the base of the haemorrhoid heals with some scar tissue.
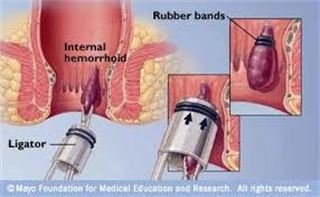
Banding is a common treatment for large internal and early prolapsing haemorrhoids. It may also be done to smaller piles which have not settled with the measures described above (increase in fibre etc).
Banding of haemorrhoids is often painless as the base of the haemorrhoid originates above the anus opening – in the very last part of the gut where the gut lining is not sensitive to pain. A small number of people have complications following banding such as urinary problems, or infection or ulcers forming at the site of a treated haemorrhoid. If the band is accidentally placed too low it can be very painful until the band drops off. Rarely, the band erodes through one of the arteries supplying a haemorrhoid and can result in a large haemorrhage requiring hospital treatment.
Generally banding is more successful than injection therapy but may at times be painful, and in more advanced cases, can require multiple applications and numerous visits to your specialist.
Formal Surgical Removal (Haemorrhoidectomy)
An operation to cut away the haemorrhoid(s) is an option to treat very large internal piles and prolapsing piles not successfully treated by banding or other methods. This is done under general anaesthetic and is usually successful at removing the piles.
It is however very painful for up to six weeks after the surgery whilst the wounds heal and patients may not return to work for many weeks. Problems with healing may also occur and many people who have undergone this operation describe the immediate post-operative period as ‘misery’.